Hip Impingement
Hip impingement is a common cause of hip pain that is a very treatable condition when it is diagnosed and recognized early. I tell my active patients with hip pain that 20 years ago hip impingement wasn’t a recognized condition and hip pain was attributed to “early hip arthritis and they would likely need a hip replacement when they get older”. That was the case until 2003 when Dr. Ganz described a condition known as FAI, or femoral acetabular impingement. FAI is a condition caused by asphericity of the femoral head, the ball of the hip socket, or over-coverage of the femoral head by the socket being too deep or angled in the wrong direction. These bony abnormalities are not mutually exclusive and most commonly occur as a combined condition of impingement. With repetitive maneuvers or activities requiring the extremes of motion the impingement causes mechanical damage to the labrum (see discussion on hip labral tears) and cartilage. This initially begins as groin pain and loss of function and if allowed to progress can lead to irreversible cartilage damage and arthritis.
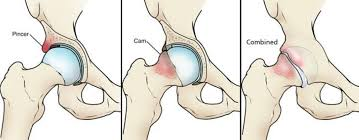
CAM type FAI is the terminology for impingement from excessive “bump” of bone on the head/neck junction of the femur. This condition is more common in males and the following are proposed causes: 1. genetic deformities occurring spontaneously 2. extremes of motion of the hip in the young athlete 3.reepetitive trauma to the growth plate of the femoral head creating a reactive bone bump 4. Slipped Capital Femoral Epiphysis (SCFE) occurring in younger kids who have an injury of the growth plate in the same location of CAM FAI. Studies have shown that athletes and adolescents participating in sports are at increased risk for this condition-as high as ten times more likely.
Pincer Type FAI refers to hip impingement caused by focal or global over-coverage of the femoral head by the socket due to the anatomy of the acetabulum-hip socket. This type of FAI is more commonly seen in women and has been attributed to genetics 10-15% of the time but is also more commonly seen in athletes as high as 55% incidence.
A third form of hip impingement can be seen in a small subset of patients known as subspine impingement. This type of impingement describes mechanical impingement of the hip in deep hip flexion with or without hip rotation that occurs due to impingement of a small bone prominence, known as the anterior inferior iliac spine (AIIS). The AIIS is located 1-2 cm above the 12 O’clock position of the socket. This normal anatomic structure is where the direct head of the quad muscle originates and it can sometimes extend to or below the rim of the socket and cause impingement in the front of the hip. Subspine impingement is typically seen in combination with other forms of hip impingement.
The presenting symptoms for FAI is a gradual onset of sharp pain or constant dull aching pain in the groin and sometimes involving the buttock that is made worse by running, jumping, squatting or prolonged sitting. The hip pain is made worse by any activity that causes flexion and simultaneous internal rotation of the hip which is when the knee is brought towards the patient’s midline. There can also be associated mechanical sx where there is popping, clicking, catching or clunking deep in the hip socket which suggests there is a labral tear in the hip.
When I suspect FAI I will get a battery of xrays in my clinic and take measurements of the bony anatomy looking for asymmetry of the joint. An important note is that there is an extremely high rate of xray abnormalities consistent with hip impingement even in patients without clinical complaints of hip pain (37% CAM and 67% Pincer). Stated another way-because you may have xrays showing hip impingement it doesn’t guarantee that impingement is the cause of the pain. I will recommend a trial of therapy, therapeutic injections and non-steroidal anti-inflammatory medications for patients with FAI, which helps relieve symptoms in the majority of patients. If that fails after a minimum of 6 weeks, I will then recommend a contrast-enhanced MRA of the hip to assess the labrum, cartilage, and any bone cysts. I sometimes obtain a 3D CT scan to look at the bony anatomy of the hip, in patients with a pincer deformity to characterize the pattern and position of the bone deformity. I utilize Stryker Arthroscopy products for my hip scopes and HIP MAP™, a pre-operative navigation program, which maps out the bone deformity for me prior to surgery. Additionally, I utilize something called HIP CHECK™ which is a computer assisted intra-operative navigation program that guides me when surgically reshaping the hip. Finally, I utilize the Guardian ™ Post-less hip arthroscopy traction table which has greatly decreased patient’s pain and the time of surgery. I encourage anybody scheduled for surgery to look at these products at Stryker.com/us
Corticosteroid injections are another non-operative intervention I use to help better pinpoint the source of hip pain as there are many other potential sources of hip pain. Injections provide temporary relief from the pain and allows patients to participate in physical therapy exercises in the attempt to avoid surgery. As a diagnostic tool, steroid injections can help localize the pain to an intra-articular source like a labral tear or cartilage damage and support the diagnosis of symptomatic FAI. Patients with clinical and radiographic evidence of FAI that improve with an intraarticular hip injection are excellent candidates for an arthroscopic surgery of the hip (hip scope).
The surgical management for FAI is a same day arthroscopic procedure done at the surgery center and typically takes about an hour. I do minimally invasive surgery with 2-3 small 2 cm incisions about the hip and I perform reshaping of the socket and/or ball as necessary using intraoperative xrays and the STRYKER HIP CHECK™ computer navigation program. I will repair the labrum as I believe it is critical to do so in order to keep the suction seal of the joint to keep the fluid lubrication intact to protect the cartilage. If the labrum is irreparable due to the complexity of the tear or in a secondary/revision surgery scenario I may recommend a labral reconstruction where I recreate an anatomic labrum from human tissue to replace the damaged labrum (see labral reconstruction Blog coming soon). I will also address any cartilage damage by cleaning it with an arthrocopic shaver, repairing it, or doing a procedure known as microfracture to heal the lesion. Literature has demonstrated nearly 90% success rate with arthroscopic management of FAI. The overall recovery is between 4-5 months to return to sports.
Not all hip impingement requires surgery and the vast majority of hip impingement on xrays is not symptomatic. The success of management of hip pain is a good history and exam and making the appropriate diagnosis. I emphasize an appropriate trial of physical therapy in patients with hip pain, limited motion and imaging consistent with FAI. One scenario where I am more proactive in discussing surgical treatment is in the setting of symptomatic FAI with a large CAM lesion. My thought process behind this philosophy of earlier surgical intervention is that by reshaping the femoral head and repairing the labrum and cartilage damage I can help slow or even prevent the progression of the disease to arthritis. I do not recommend prophylactic correction of the other hip in patients with bilateral FAI unless they develop pain in the contralateral hip-the old adage don’t fix it if it isn’t broken. Hip arthroscopy has become a very predictable means of treating FAI with minimally invasive surgery and I would be honored to take care of your hip pain with the most cutting-edge technology and surgical techniques in hip arthroscopy.